By Hira Waheed1, Zishan Haider1, Owais Rao1, Syed Jahanzeb2
AFFLIATIONS:
- Department of Radiology, Aga Khan University Hospital, Karachi, Pakistan.
- Department of Orthopedic, Civil Hospital, Karachi, Pakistan.
DOI: https://doi.org/10.36283/PJMD11-3/013
ORCID iD: 0000-0002-6221-7446
How to cite: Waheed H, Haider Z, Rao O, Jahanzeb S. Periampullary Carcinoma in Pregnancy – A Rare Cause of Jaundice in Pregnant Population. Pak J Med Dent. 2022;11(3): 82-85. doi: 10.36283/PJMD11-3/013
Periampullary carcinoma is one of the rarest cancers worldwide and causes >30,000 deaths annually in the United States (US). These cancers arise in close approximation to the papilla of Vater and include tumors of the distal common bile duct, ampullary region, duodenum, and pancreas. The clinical characteristics and curative approaches of the periampullary tumor spectrum are almost similar; however, their long-term outcomes are generally different. In this report, a case of periampullary adenocarcinoma was presented, diagnosed during the first trimester of a woman. As it is quite a rare entity in pregnancy, it should be suspected when patients complain of epigastric pain and jaundice with laboratory parameters suggestive of biliary tract obstruction during pregnancy to avoid misdiagnosis. The need to optimize both maternal and fetal outcomes is essentially challenging when surgical interventions are required for staging and various therapeutic purposes.
Keywords: Pregnancy; Magnetic Resonance Imaging; Endoscopic Retrograde Cholangiopancreatography.
Periampullary carcinoma is one of the rarest and most lethal cancer1. It has resulted in >30,000 deaths annually in the United States 2. These arise in close approximation to the papilla of Vater and include carcinomas of the distal common bile duct (CBD), ampullary region, duodenum, and pancreas. The clinical characteristics and curative approaches of the periampullary tumor spectrum are almost similar; however, their long-term outcomes are generally variable3. Its prevalence in young patients is infrequent and even rare during pregnancy4. The need to improve both maternal and fetal outcomes is challenging when surgical interventions are needed for therapeutic purposes.
A 31-year-old lady (G2P1) presented at 6 weeks gestational age, with an insignificant past medical history. She came with occasional fever, jaundice, and undocumented weight loss for the last two months. She was initially treated on the lines of enteric fever, starting with ceftriaxone and metronidazole. Her total serum bilirubin was 0.6 mg/Dl, serum direct bilirubin was 0.3 mg/Dl with an alkaline phosphatase of 559 IU/L. Her ultrasound abdomen, magnetic resonance cholangiopancreatography (MRCP), and Computed Tomography (CT) showed cholelithiasis. Soft tissue thickening in the distal common bile duct which is resulting in moderately dilated proximal CBD and moderate intrahepatic biliary dilatation. However, no calculus was noted in the CBD. An endoscopic retrograde cholangiopancreatography (ERCP) was done subsequently with appropriate shielding and radiation protection, which showed stricture in the distal CBD consistent with extrinsic compression from a peripancreatic mass. Papillotomy and biliary stenting were performed. ERCP brushings revealed poorly differentiated adenocarcinoma of the periampullary region. The CT scan further showed the absence of metastatic disease.
Her family was counseled and it was planned to terminate her viable pregnancy on medical grounds. Ten days following her dilation and evacuation (D&E), the patient underwent an uncomplicated pancreatoduodenectomy (Whipple’s procedure). The surgical findings showed a periampullary mass with a few benign-appearing peripancreatic lymph nodes. CBD was thick-walled. No ascites or peritoneal disease was seen. A feeding jejunostomy was made. The patient recovered well in the postoperative period. The histopathological report revealed a 1.5 x 1.5 cm poorly differentiating adenocarcinoma in the periampullary location which is infiltrating through the mucosa into the muscularis propria and focal extension into the adjacent CBD. The proximal, distal bile duct, pancreatic and retroperitoneal margins are tumor-free. Multiple peripancreatic and aortocaval lymph nodes were also tumor-free. The TNM staging (T2 N0 MX) made it a stage IB periampullary carcinoma (Figure 1). The next step in the management was chemotherapy and radiation. She received gemcitabine and 5FU. During her course of chemotherapy, she once developed neutropenic fever/ myelosuppression secondary to gemcitabine, for which she was conservatively managed.
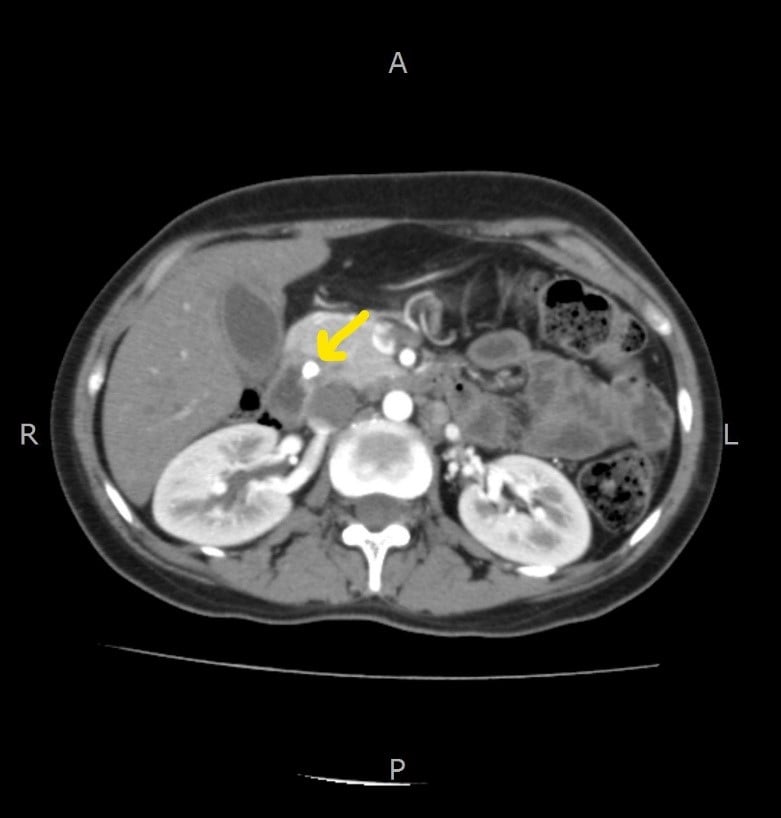
Figure 1: Contrast-enhanced CT Abdomen showing soft tissue thickening in the periampullary location close to the distal common bile duct (CBD).
The periampullary and pancreatic malignancies that have been diagnosed during pregnancy with histopathological confirmation are found rare in the literature. To the best of the knowledge, only 42 cases have been reported by 2019 and this case is the 43rd 5. Porcel et al. published the first case of adenocarcinoma of the ampulla of Vater in a pregnant woman in her last trimester in 1992 6. The most common age of presentation was in the 30s, same in this case as well. The most common histopathological type was identified to be adenocarcinoma (18 cases) followed by mucinous cystic neoplasm (16 cases), and neuroendocrine neoplasms (3 cases), solid-pseudopapillary neoplasms (3 cases) and anaplastic (1 case).
In this case, the possible cause of biliary obstruction in a 31-year-old lady is common bile duct calculi. The complete evaluation of jaundice during pregnancy requires additional importance. In addition to the clinical presentation and baseline pathological investigations, advanced radiological tests are necessitated to exclude distal CBD calculi or neoplastic lesions of the ampulla/ periampullary, pancreatic, or biliary duct origin. The attempt to perform an ERCP, in this case, had risks associated with radiation to the fetus. But the decision had to be taken to assess risk versus benefit to the patient. Subsequently, taking the patient’s condition into account, MRCP and ERCP were performed which revealed periampullary carcinoma. Careful and adequate tumor staging of periampullary carcinoma was extremely important in categorizing patients who would benefit from attempting a pancreatoduodenectomy with curative intent. The preoperative assessment should include investigations that are sensitive and specific for detecting localized and relatively curable diseases and identifying locally advanced and metastatic diseases which may render the tumor unresectable2.
Various diagnostic methods for staging are important to provide information on tumor location and size, the presence of extrahepatic tumor involvement, hepatic metastases, peritoneal carcinomatosis, or ascites. Moreover, the presence of regional retroperitoneal lymph nodal involvement (periportal, peripancreatic, celiac, or superior mesenteric), vascular encasement, infiltration, and involvement should also be mentioned2. An incidence of 30-50% lymph nodal metastasis has been reported in periampullary tumors7. Perineural invasion is also a very important characteristic and usually embarks a poor prognosis, being reported in 5-17 % of patients7.
It is relatively challenging to radiologically assess the periampullary region owing to its anatomical location in the retroperitoneum and its relation with surrounding abdominal viscera and their major abdominal vasculature. Although useful but radiological investigations like ultrasound, CT scan, magnetic resonance imaging, and selective visceral angiography may not always be 100% accurate in the staging of these carcinomas. However, endoscopic ultrasound and helical or spiral CT, in recent times have demonstrated extremely good accuracy in diagnosing small periampullary tumors, their metastatic lymph nodal status, and hepatic metastatic lesions.
The primary management step, in this case, was to relieve biliary obstruction through stenting. Although the periampullary tumor spectrum shares common clinical presentation, anatomy, and surgical management options (classic or pylorus-preserving pancreaticoduodenectomy), their long-term outcomes may differ according to a specific type of tumor. The overall survival rate is much better for patients with ampullary/ periampullary cancers, intermediate/borderline for patients with bile duct carcinoma, and lowest for patients with a pancreatic tumor7,8. The operative rate for periampullary tumors is also much better than that for pancreatic ductal adenocarcinoma. It is reported to be 80% in comparison to 15% for pancreatic head cancer 2,9,10. Classic or pylorus-preserving pancreatoduodenectomy is the surgical procedure of choice for the periampullary neoplastic disease spectrum in patients with resectable disease. This technique is now gaining popularity and is a standard surgery for periampullary neoplasm2. The 5-year survival rates have shown a progressive improvement over time after surgical resection.
The maximum survival rates after pancreatoduodenectomy have been reported with ampullary and duodenal tumors. Several other factors also affect the overall survival rate of periampullary tumors. These comprise the size of the tumor (< 3 cm), regional lymph nodal metastases, perineural invasion, and degree of differentiation after surgical resection2. In patients with unresectable tumors, having biliary or gastric outlet obstruction, palliative bilio-digestive bypass procedures are usually recommended. A choledochojejunostomy or a cholecystojejunostomy combined with a gastrojejunostomy is the surgery of choice with excellent long-term results, and improved morbidity and mortality rates11,12. Recent clinical trials involving chemotherapeutic agents like concurrent 5-fluorouracil (5-FU), dipyridamole (DPM), leucovorin (LV), and mitomycin-C (MMC) combined with split-course loco-regional external beam radiotherapy (EBRT) to 50Gy have demonstrated good clinical outcomes13.
Because the cancers increase with pregnancy, pain and laboratory parameters suggest an appropriate evaluation, and management plan should be implemented and modified on an individual case basis. There should be avoidance of inadequate generalizations. An effective treatment plan should be followed, particularly for specific cancer, and addressing the risk factors and side effects associated with each following the fetal gestational age.
The authors would like to acknowledge hospital staff and doctors for their immense contribution.
It is confirmed that all authors of the manuscript have no conflict of interest to declare.
This is not applicable as only the retrospective data was used to write the manuscript.
The clinicians obtained the patient consent.
HW was a major contributor in compiling the data and writing the manuscript. ZH contributed to the case diagnosis. OR helped with the data collection, and SJ assisted in analyzing and finalizing the manuscript.
- American Cancer Society, Inc. American Cancer Society: Cancer Facts and Figures [Internet]. 2010: Page 4 [cited 2022 Mar 10]. Available from: http://www.cancer.org/acs/groups/content/@nho/document/acspc-024113.pdf
- Fernandez-Cruz L. Periampullary carcinoma. In: Holzheimer RG, Mannick JA, editors. Surgical Treatment: Evidence-Based and Problem-Oriented. Munich: Zuckschwerdt; 2001. Available from: https://www.ncbi.nlm.nih.gov/books/NBK6924/
- Kim JH, Kim MJ, Chung JJ, Lee WJ, Yoo HS, Lee JT. Differential diagnosis of periampullary carcinomas at MR imaging. Radiographics. 2002;22(6):1335-1352. doi: 10.1148/rg.226025060
- Donegan WL. Cancer and pregnancy. CA Cancer J Clin. 1983;33(4):194-214. doi: 10.3322/canjclin.33.4.194
- AlQattan AS, Alkuwaiti FA, Alghusnah ES, Bojal SA, Alqahtani MS. Challenges in the management of adenocarcinoma of ampulla of Vater in pregnancy: A case report and review of literature. Int J Surg Case Rep. 2019;61:38-43. doi: 10.1016/j.ijscr.2019.06.044
- Porcel JM, Ordi J, Castells L, Farran I. Probable pancreatic cancer in a pre-eclamptic patient. Eur J Obstet Gynecol. 1992;44(1):80-82.
- Jagannath P, Shrikhande S. Current options in the diagnosis and management of periampullary carcinoma. Indian J Surg. 2003;65:347-53.
- Chan C, Herrera MF, de la Garza L, Quintanilla-Martinez L, Vargas-Vorackova F, Richaud-Patin Y, et al. Clinical behavior and prognostic factors of periampullary adenocarcinoma. Ann Surg. 1995; 222(5): 632-637. doi: 10.1097/00000658-199511000-00005
- Ihse I, Andrén-Sandberg Å, Permerth J, Larsson J. Early results of subtotal pancreatectomy for cancer: An interim report. In Standards in pancreatic surgery 1993 (pp. 641-645). Springer, Berlin, Heidelberg. Available from: https://link.springer.com/chapter/10.1007/978-3-642-77437-9_71
- Ihse I, Larsson J. Periampullary lesions. Cancer of the Bile Duct and the Pancreas. London: WB Saunders. 1989:83-91.
- Yamaguchi K, Kishinaka M, Nagai E, Nakano K, Ohtsuka T, Chijiwa K, et al. Pancreatoduodenectomy for pancreatic head carcinoma with or without pylorus preservation. Hepatogastroenterology. 2001;48(41):1479-1485.
- Sohn TA, Lillemoe KD, Cameron JL, Huang JJ, Pitt HA, Yeo CJ. Surgical palliation of unresectable periampullary adenocarcinoma in the 1990s. J Am Coll Surg. 1999;188(6):658-666. doi: 10.1016/S1072-7515(99)00049-6
- Chakravarthy A, Abrams RA, Yeo CJ, Korman LT, Donehower RC, Hruban RH, Zahurek ML, Grochow LB, O’Reilly S, Hurwitz H, Jaffee EM. Intensified adjuvant combined modality therapy for resected periampullary adenocarcinoma: acceptable toxicity and suggestion of improved 1-year disease-free survival. Int J Radiat Oncol Biol Phys. 2000;48(4):1089-1096. doi: 10.1016/S0360-3016(00)00755-0
This is an open-access article distributed under the terms of the CreativeCommons Attribution License (CC BY) 4.0 https://creativecommons.org/licenses/by/4.0/
